Has laparoscopic approach replaced the open technique to perform appendectomy?—evolution over more than a decade
Introduction
Acute appendicitis is the most common surgical emergency requiring early operative intervention (1-3). Approximately 8% of the population suffers from acute appendicitis during the second and third decade of life (4,5), with slight male preponderance (1). Appendectomy remains the recommended treatment for patients suffering from acute appendicitis. With advent of laparoscopic approach to abdominal surgical problems, laparoscopic appendectomy has also progressively gained popularity since 1982 when it was performed first time by Semm et al. (6-9).
Better cosmetic outcomes, rapid recovery, short hospital stay, fewer complications and less narcotic requirement are among the advantages of laparoscopic approach over open technique (10,11). However, unlike laparoscopic cholecystectomy that attained the status of “standard of care” in a very short time span, laparoscopic appendectomy is yet to find that place (12).
Lack of laparoscopic surgical expertise and relatively high cost have hindered the adoption of laparoscopic approaches especially in developing countries (13). The Aga Khan University Hospital (AKUH) in Karachi, Pakistan introduced laparoscopy in 1990 and the first laparoscopic cholecystectomy was performed in 1992. However, it was not until 2004 that the first laparoscopic appendectomy was performed. At present, laparoscopy is the preferred approach for appendectomy and standard for cholecystectomy.
Objective(s)
To report adaptation trends of laparoscopic appendectomy over a period of 12 years and lessons learnt from it.
Methods
We conducted retrospective cohort study at Department of Surgery at the Aga Khan University Hospital (AKUH) Karachi. AKUH is a 650-bed tertiary care hospital with seven general surgeons credentialed to perform laparoscopic appendectomy.
Selection criteria
All adult patients of age 16 years and above, admitted with acute appendicitis and underwent laparoscopic appendectomy from January 01, 2004 to December 31, 2015 were included in the study. Patients with missing data, incomplete records and those who underwent two simultaneous procedures were excluded from the study.
Data collection procedure
Medical records of patients included in the study were retrieved using International Classification of Disease (ICD) codes. The data was collected on a specifically designed questionnaire. Demographics like age, gender, comorbidities, length of stay, radiological workup, type of surgery (laparoscopic or laparoscopic converted to open), reason for conversion, operative findings, duration of surgery, post-operative complications and histopathological findings were recorded. Approval was sought from institutional review board before start of the study. Approval number granted is 3748-Sue-ERC-15.
Statistical analysis
Data was entered and analyzed using SPSS version 22. Qualitative variables are reported as numbers, percentages or proportions. Quantitative variables are reported as means with standard deviations or medians with inter-quartiles ranges depending upon the distribution of data. Chi-square test was used to compare qualitative variables across the groups while ANOVA was applied to compare quantitative variable. P value of <0.05 was considered as statistically significant.
Results
A total of 1,163 patients underwent laparoscopic appendectomy during the study period out of which 831 met inclusion criteria while 332 were excluded based on the exclusion criteria. About 2/3rd (64.0%) of our patients were males. The median age of our patients was 28 years (IQR, 22–37). Baseline characteristics of patients are as given in Table 1.
Table 1
| Variables | Overall | 2004–2007 | 2008–2011 | 2012–2015 | P value |
|---|---|---|---|---|---|
| Number (%) | 831 | 98 (11.8) | 331 (39.8) | 402 (48.4) | |
| Gender | 0.22 | ||||
| Male, n (%) | 532 (64.0) | 57 (58.2) | 207 (62.5) | 268 (66.7) | |
| Female, n (%) | 299 (36.0) | 41 (41.8) | 124 (37.5) | 134 (33.3) | |
| Diabetes mellitus, n (%) | 37 (4.5) | 4 (4.1) | 12 (3.6) | 21 (5.2) | 0.57 |
| Age (years), mean ± SD | 30.8±12.1 | 31.2±12.4 | 30.1±11.6 | 31.4±12.4 | 0.35 |
| Duration of symptom (days), mean ± SD | 1.6±1.0 | 1.6±1.1 | 1.6±1.1 | 1.6±0.9 | 0.89 |
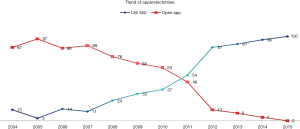
Proportion of patients who underwent laparoscopic appendectomy as opposed to open surgery increased over time. In 2004 only 13% of the cases were attempted laparoscopically while this proportion was 100% in 2015 (P<0.001). Year wise details are as shown in Figure 1.
Of all the cases attempted laparoscopically, conversion to open was done in 7% [59] cases mainly due to dense adhesions of the appendix to surrounding structures resulting in difficult anatomy. Perforation at the base of appendix accounted for conversion to open in 5 cases while two cases were converted to open surgery because of iatrogenic injuries. The conversion rate, however, decreased over the years from 10.2% in initial 4 years to 5% in last 4 years of study duration (P=0.062).
Mean duration of surgery was 64.5 (+/−23) minutes. A statistically significant (P<0.001) decrease in duration of surgery was noticed, from the mean of 74 minutes in initial 4 years to the mean of 60.5 minutes in last 4 years of the study period. Overall negative appendectomy rate was 7.82%. Similar to other findings, results demonstrated a falling trend in negative appendectomy rates from 22.4% in initial 4 years to 4.98% in last 4 years of the study period (P<0.001). Details of the results are as shown in Table 2.
Table 2
| Variables | Overall | 2004–2007 | 2008–2011 | 2012–2015 | P value |
|---|---|---|---|---|---|
| Number (%) | 831 | 98 (11.8) | 331 (39.8) | 402 (48.4) | |
| Operative duration (min) | 64.5±23 | 74 | 67 | 60.5 | 0.001 |
| Conversion, % (N) | 7 [59] | 10.2% | 8.8% | 5% | 0.062 |
| Negative appendectomies, % (N) | 7.82 [65] | 22.4% | 6.94% | 4.98% | <0.001 |
| Overall complications, % (N) | 6.37 [53] | 4.6% | 2.5% | 10.9% | <0.001 |
Surgical site infection was the most common post-operative complication affecting 4.5% [37] of our patients; this included 19 (2.28%) patients with intra-abdominal abscess. Re-admission rate was 1.6% (13). Only two patients required redo surgery for intra-abdominal collection wash out while rest of patients were managed by drain placement radiologically.
Discussion
Appendectomy is the standard of care for acute appendicitis. The laparoscopic approach is becoming the preferred way among an increasing number of surgeons worldwide, though the open technique is still more common because of its low cost and shorter duration of surgery (14,15). Furthermore, change in surgical practice depends upon multitude of factors in addition to cost and skills (16).
Duration of surgery is an important determinant of surgical outcomes. Studies have shown that laparoscopic appendectomy takes much longer than open technique (17,18). This factor keeps the laparoscopic technique from becoming the standard of care. As the experience of a surgeon increases, the duration of operation decreases (13). Our findings are in synchrony with this argument, since over time the duration of laparoscopic appendectomies performed at our institute has decreased significantly. The mean duration of surgery is 64.5 minutes which is comparable to that illustrated by the study done by Kouhia et al. (19).
The rate of conversion from laparoscopic to open appendectomy is another area that has direct impact on surgical outcomes. Our data showed that 7% of the cases were converted to open technique which is comparable to the rate demonstrated in another study (19). However, our conversion rate is much higher than the rate reported by the study done by Bozkurt et al. in Istanbul, Turkey and this can be explained by the fact that Bozkurt et al. excluded all complicated cases of appendicitis (20). Our trend shows a consistent improvement in conversion rate (21).
Superiority of laparoscopic appendectomy to open appendectomy has consistently been reported so far as early post-operative pain, length of hospital stays and early return to work is concerned. Recent meta-analysis by Jaschinski et al. also confirmed that post-operative pain, length of hospital stays, wound infection, return to work and quality of life are improved after laparoscopic appendectomy as compared to open appendectomy (22). However, risk of post-operative intra-abdominal abscess formation especially after appendectomy for complicated appendicitis is high after laparoscopic appendectomy than open approach (22,23). Risk of intra-abdominal abscess formation was only 1.10% in multicenter cohort study reported by Lasek et al. Complicated appendicitis was the only predictive factor for post-operative intra-abdominal abscess formation (24). In this sub-group of patients with ruptured or gangrenous appendicitis open approach may be superior due to ability to give a through wash out during operation.
Despite proven advantages of laparoscopic appendectomy over open surgery for uncomplicated appendicitis, open appendectomy is still offered frequently as first treatment option. Multiple factors are involved in resistance to change in surgical practice. Lack of resources, lack of skills, cost of care, mistaken beliefs of non-superior outcome, operative duration and lack of external validity of certain technique are few of the factors involved. Recent survey of Polish surgeon about their awareness and practice of laparoscopic hernia repair reported that 19.2% do not inform patients about laparoscopic repair option and 61.6% surgeon perform staged open repair of bilateral inguinal hernia (25). These factors result in dissonance between evidence and practice (16).
Conclusions
Laparoscopic appendectomy has potential to replace open technique as treatment option for acute appendicitis given the advantages of laparoscopic surgery especially for uncomplicated appendicitis.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/ales.2019.04.08). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). Approval was sought from institutional ethical review board before start of study. Approval number is 3748-SUR-ERC-15. Informed consent was taken from all individual participants.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Addiss DG, Shaffer N, Fowler BS, et al. The epidemiology of appendicitis and appendectomy in the United States. Am J Epidemiol 1990;132:910-25. [Crossref] [PubMed]
- Zhang Y, Zhao YY, Qiao J, et al. Diagnosis of appendicitis during pregnancy and perinatal outcome in the late pregnancy. Chin Med J 2009;122:521-4. [PubMed]
- Ozguner IF, Buyukayavuz BI, Savas MC. The influence of delay on perforation in childhood appendicitis. A retrospective analysis of 58 cases. Saudi Med J 2004;25:1232-6. [PubMed]
- Kumar B, Samad A, Khanzada TW, et al. Superiority of laparoscopic appendectomy over open appendectomy: the Hyderabad experience. Rawal Med J 2008;33:165-8.
- Fahim F, Shirjeel S. A comparison between presentation time and delay in surgery in simple and advanced appendicitis. J Ayub Med Coll Abbottabad 2005;17:37-9. [PubMed]
- Eriksson S, Granström L. Randomized controlled trial of appendicectomy versus antibiotic therapy for acute appendicitis. Br J Surg 1995;82:166-9. [Crossref] [PubMed]
- Semm K. Endoscopic appendectomy. Endoscopy 1983;15:59-64. [Crossref] [PubMed]
- Milewczyk M, Michalik M, Ciesielski M. A prospective, randomized, unicenter study comparing laparoscopic and open treatments of acute appendicitis. Surg Endosc 2003;17:1023-8. [Crossref] [PubMed]
- Sweeney KJ, Keane FB. Moving from open to laparoscopic appendicectomy. Br J Surg 2003;90:257-8. [Crossref] [PubMed]
- Rashid A, Nazir S, Kakroo SM, et al. Laparoscopic interval appendectomy versus open interval appendectomy: a prospective randomized controlled trial. Surg Laparosc Endosc Percutan Tech 2013;23:93-6. [Crossref] [PubMed]
- Yaghoubian A, Kaji AH, Lee SL. Laparoscopic versus open appendectomy: outcomes analysis. Am Surg 2012;78:1083-6. [PubMed]
- Hori T, Oike F, Furuyama H, et al. Protocol for laparoscopic cholecystectomy: Is it rocket science? World J Gastroenterol 2016;22:10287. [Crossref] [PubMed]
- Bennett J, Boddy A, Rhodes M. Choice of approach for appendicectomy: a meta-analysis of open versus laparoscopic appendicectomy. Surg Laparosc Endosc Percutan Tech 2007;17:245-55. [Crossref] [PubMed]
- Bachar I, Perry ZH, Dukhno L, et al. Diagnostic value of laparoscopy, abdominal computed tomography, and ultrasonography in acute appendicitis. J Laparoendosc Adv Surg Tech A 2013;23:982-9. [Crossref] [PubMed]
- Karamanakos SN, Sdralis E, Panagiotopoulos S, et al. Laparoscopy in the emergency setting: a retrospective review of 540 patients with acute abdominal pain. Surg Laparosc Endosc Percutan Tech 2010;20:119-24. [Crossref] [PubMed]
- Shahzad N, Chawla TU, Begum S, et al. Pancreaticojejunostomy versus pancreaticogastrostomy after pancreaticoduodenectomy to prevent post-operative pancreatic fistula, a dissonance between evidence and practice. Arch Clin Gastroenterol 2018;4:008-11.
- Ali R, Khan MR, Pishori T, et al. Laparoscopic appendectomy for acute appendicitis: Is this a feasible option for developing countries? Saudi J Gastroenterol 2010;16:25. [Crossref] [PubMed]
- Jaschinski T, Mosch C, Eikermann M, et al. Laparoscopic versus open appendectomy in patients with suspected appendicitis: a systematic review of meta-analyses of randomised controlled trials. BMC Gastroenterol 2015;15:48. [Crossref] [PubMed]
- Kouhia ST, Heiskanen JT, Huttunen R, et al. Long-term follow-up of a randomized clinical trial of open versus laparoscopic appendicectomy. Br J Surg 2010;97:1395-400. [Crossref] [PubMed]
- Bozkurt MA, Unsal MG, Kapan S, et al. Is laparoscopic appendectomy going to be standard procedure for acute appendicitis; a 5-year single center experience with 1,788 patients. Eur J Trauma Emerg Surg 2015;41:87-9. [Crossref] [PubMed]
- van Rossem CC, Bolmers MD, Schreinemacher MH, et al. Prospective nationwide outcome audit of surgery for suspected acute appendicitis. Br J Surg 2016;103:144-51. [Crossref] [PubMed]
- Jaschinski T, Mosch CG, Eikermann M, et al. Laparoscopic versus open surgery for suspected appendicitis. Cochrane Database Syst Rev 2018;11:CD001546 [PubMed]
- Li X, Zhang J, Sang L, et al. Laparoscopic versus conventional appendectomy-a meta-analysis of randomized controlled trials. BMC Gastroenterol 2010;10:129. [Crossref] [PubMed]
- Lasek A, Pędziwiatr M, Wysocki M, et al. Risk factors for intraabdominal abscess formation after laparoscopic appendectomy–results from the Pol-LA (Polish Laparoscopic Appendectomy) multicenter large cohort study. Wideochir Inne Tech Maloinwazyjne 2019;14:70. [Crossref] [PubMed]
- Mitura K, Dąbrowiecki S, Śmietański M, et al. The experience and awareness of laparoendoscopic procedures among Polish surgeons in everyday clinical practice. Wideochir Inne Tech Maloinwazyjne 2017;12:13. [Crossref] [PubMed]
Cite this article as: Siddiqui MTUH, Sultan R, Zafar H, Bhatti UF, Shaukat F, Shahzad N. Has laparoscopic approach replaced the open technique to perform appendectomy?—evolution over more than a decade. Ann Laparosc Endosc Surg 2019;4:48.