
The advantage of intracorporeal techniques
Introduction
Since its inception there has been an increasing usage of minimally invasive surgery for the treatment of colon and rectal disease. In that time, multiple studies have demonstrated the safety and efficacy of laparoscopic surgery for the treatment of both benign and malignant diseases of the colon and rectum (1-6). Advantages of minimally invasive surgery have been described as decreased postoperative pain and narcotic usage, decreased postoperative hospital length of stay, early return of bowel function, quicker return to work, and decreased postoperative incisional hernia risk. In this article we will look beyond the benefits of laparoscopic surgery and focus specifically on the benefits of performing an intracorporeal anastomosis during colon surgery.
In bariatric surgery, a significant leap was made in the transition from open roux-en-y gastric bypass to the development of laparoscopic roux-en-y gastric bypass. Laparoscopic gastric bypass surgery requires multiple intracorporeal anastomoses in each procedure. Surgeons faced a significant learning curve to make that adjustment but today laparoscopic approach to gastric bypass, and other bariatric surgeries, remains the standard of care (7,8). Laparoscopic colon and rectal surgery has also made significant advances since its early days. Interestingly though, descriptions of laparoscopic colon and rectal surgery still include incisions large enough to facilitate specimen extraction, use of a hand port for hand-assisted techniques, or a combination of laparoscopic and open approach for pelvic dissection. Furthermore, many surgeons continue to preferentially perform extracorporeal anastomoses to reestablish intestinal continuity after segmental resection.
Advocates for extracorporeal anastomosis argue that the need for a specimen extraction site makes this technique equivalent to intracorporeal anastomosis. Unfortunately, the choice to perform an extracorporeal anastomosis may negatively influence the chosen site of extraction. Given midline incisions have increased rates of incisional hernia development, the ability to select an extraction site other than the midline can confer significant long term benefits to the patient (9-11).
The wide array of techniques and operative approaches that live under the minimally invasive umbrella of colon and rectal surgery may also influence the benefits of laparoscopic surgery when compared with open techniques. Factors such as postoperative length of stay, postoperative ileus rates, and patient satisfaction, may all be influenced by opting for a totally laparoscopic technique with intracorporeal anastomosis. In this article we will discuss the intracorporeal anastomosis, its operative technique, its benefits, and how the technique compares to extracorporeal anastomosis with regards to postoperative outcomes.
Anastomotic leak
Anastomotic construction is a critical part of every colon and rectal operation. Anastomotic leak rates in colon and rectal surgery are described as ranging from 1–3% for ileocolic anastomoses, and has been described as upwards of 20% for colorectal anastomoses (12,13). Anastomotic leak is a fretted complication and this is likely a contributing factor for the reluctance of surgeons to make the jump to performing an intracorporeal anastomosis in laparoscopic colorectal surgery. Many can be wary of altering such a critical aspect of a surgery. Also, with the ability to position an extraction incision in location to facilitate extracorporeal anastomosis, most surgeons do not see a need for making such a transition.
Anastomotic leak rates have been shown to be comparable between open and laparoscopic surgery for colon resections (1,3). Though, as described above, in many of these trials, an extracorporeal anastomosis is performed. Multiple smaller scale investigations have been performed to investigate intracorporeal vs. extracorporeal anastomoses and have demonstrated no difference in leak rates between the two techniques (14-17). Lack of comfortability with intracorporeal stapling and suturing may be a factor in the relatively slow adoption of intracorporeal anastomotic technique. It appears that in experienced hands intracorporeal anastomotic construction has, at a minimum, equivalent leak rates compared with open techniques.
Incisional hernia
Incisional hernias after colectomy are a common complication, which cause significant morbidity and whose risk can be mitigated by opting for a totally laparoscopic technique with an intracorporeal anastomosis. Incisional hernia rates after laparoscopic colorectal surgery can occur in upwards of 30% of patients (10). It is clear that laparoscopic approach alone does not mitigate the risk of incisional hernia. The lack in reduction is possibly due to surgeons opting to perform an extracorporeal anastomosis through a midline incision. Unfortunately, unless a colorectal anastomosis is planned, midline incisions are often used for extraction and extracorporeal anastomosis. Midline incisions are associated with significantly increased rates of incisional hernia when compared with incisions made off the midline, especially Pfannenstiel incisions (9-11). Currently, a prospective multi-institutional study is ongoing to investigate incisional hernia rates following intracorporeal and extra-corporeal anastomosis in laparoscopic and robotic right colectomies.
Natural orifice extractions, either transvaginal or transanal, also can help minimize incisional hernia risk. These extractions allow for a totally laparoscopic approach with no incisions aside from port site incisions. In appropriately selected patients these natural orifice extractions have been shown to be safe and feasible (18,19). The ability to forgo a midline incision, or any incision for that matter, is a significant advantage to any patient undergoing laparoscopic colectomy.
Overall, it appears a major factor in avoiding a postoperative incisional hernia is a critical evaluation of the extraction site, should one be necessary. Intracorporeal anastomosis allows for all extraction sites to be considered while extracorporeal anastomosis limits the choice of extraction site to one that facilitates exposure of the operative field.
Surgical site infections
Surgical site are a commonly addressed problem in colon and rectal surgery and significant work has been aimed at reducing surgical site infections following colectomy. Habits aimed at preserving sterility during clean contaminated cases such as the use of closing trays, changing gloves and gowns after anastomotic construction, and use of incisional wound protectors, have been associated with decreased rates of surgical site infections. Currently, intracorporeal and extracorporeal anastomoses appear to have equivalent rates of both deep and superficial surgical site infections (14,15,20).
Postoperative recovery
Laparoscopic colorectal resections have been associated with improved short term patient outcomes. Rates of postoperative ileus, time to flatus, and time to hospital discharge have all been shown to improve with laparoscopic approaches. Intracorporeal anastomosis is associated with improvements beyond what is achieved by extracorporeal anastomosis in some series. Both single and multi-institution experiences have shown improved rates of return of bowel function and shortened hospital length of stay when comparing intracorporeal and extracorporeal anastomosis, however this is not seen in all series investigating the two techniques (20,21).
Techniques
Iso-peristaltic ileocolic anastomosis (Figure 1)

Prior to creating the anastomosis the mesentery is divided at the planned transection location, ileum and colon are divided with linear staplers, and the specimen is set aside for later extraction. The limbs of the ileum and colon are aligned in an isoperistaltic configuration in the right upper quadrant. A traction suture is placed through the antimesenteric taenia of the colon and the staple line of the ileum. Next, enterotomies are created using an energy device and a laparosocpic linear stapler is employed to create the common channel of the anastomosis. The common enterotomy is typically sutured closed using an absorbable suture as to not narrow the efferent limb of the anastomosis.
Anti-peristaltic ileocolic anastomosis (Figure 2)
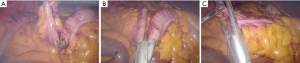
When performing an anti-peristaltic anastomosis the ileum and colon are oriented so that both staple lines align. The traction suture is placed through each staple line towards the antimesenteric edge of the bowel Next, enterotomies are created adjacent to the traction suture and again a linear stapler is used to create the common channel of the anastomosis. The common enterotomy can then be closed with either a linear stapler or laparoscopic suturing, whichever the surgeons preference.
Conclusions
Intracorporeal anastomotic construction is a technique which is safe and confers multiple benefits to patients undergoing colon and rectal surgery. The actual anastomotic construction techniques mirror the techniques used for extracorporeal anastomosis, though experience with advanced laparoscopy is needed. The largest benefits are likely the decreased risk of postoperative incisional hernia and a prospective multicenter trial investigating this outcome is underway.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Michael J Stamos and Mehraneh Dorna Jafari) for the series “Laparoscopic Colon Surgery” published in Annals of Laparoscopic and Endoscopic Surgery. The article has undergone external peer review.
Conflicts of Interest: The author has completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/ales.2018.12.08). The series “Laparoscopic Colon Surgery” was commissioned by the editorial office without any funding or sponsorship. The author has no other conflicts of interest to declare.
Ethical Statement: The author is accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Clinical Outcomes of Surgical Therapy Study Group. A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med 2004;350:2050-9. [Crossref] [PubMed]
- Braga M, Frasson M, Vignali A, et al. Laparoscopic vs. open colectomy in cancer patients: long-term complications, quality of life, and survival. Dis Colon Rectum 2005;48:2217-23. [Crossref] [PubMed]
- Guillou PJ, Quirke P, Thorpe H, et al. Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. Lancet 2005;365:1718-26. [Crossref] [PubMed]
- Fleshman J, Branda ME, Sargent DJ, et al. Disease-free Survival and Local Recurrence for Laparoscopic Resection Compared With Open Resection of Stage II to III Rectal Cancer: Follow-up Results of the ACOSOG Z6051 Randomized Controlled Trial. Ann Surg 2018; [Epub ahead of print]. [Crossref] [PubMed]
- van der Pas MH, Haglind E, Cuesta MA, et al. Laparoscopic versus open surgery for rectal cancer (COLOR II): short-term outcomes of a randomised, phase 3 trial. Lancet Oncol 2013;14:210-8. [Crossref] [PubMed]
- Jeong SY, Park JW, Nam BH, et al. Open versus laparoscopic surgery for mid-rectal or low-rectal cancer after neoadjuvant chemoradiotherapy (COREAN trial): survival outcomes of an open-label, non-inferiority, randomised controlled trial. Lancet Oncol 2014;15:767-74. [Crossref] [PubMed]
- Nguyen NT, Wolfe BM. Laparoscopic Versus Open Gastric Bypass. Semin Laparosc Surg 2002;9:86-93. [Crossref] [PubMed]
- Luján JA, Frutos MD, Hernández Q, et al. Laparoscopic Versus Open Gastric Bypass in the Treatment of Morbid Obesity: A Randomized Prospective Study. Ann Surg 2004;239:433-7. [Crossref] [PubMed]
- Singh R, Omiccioli A, Hegge S, et al. Does the extraction-site location in laparoscopic colorectal surgery have an impact on incisional hernia rates? Surg Endosc 2008;22:2596-600. [Crossref] [PubMed]
- Lee L, Mappin-Kasirer B, Sender Liberman A, et al. High incidence of symptomatic incisional hernia after midline extraction in laparoscopic colon resection. Surg Endosc 2012;26:3180-5. [Crossref] [PubMed]
- DeSouza A, Domajnko B, Park J, et al. Incisional hernia, midline versus low transverse incision: what is the ideal incision for specimen extraction and hand-assisted laparoscopy? Surg Endosc 2011;25:1031-6. [Crossref] [PubMed]
- Eto K, Urashima M, Kosuge M, et al. Standardization of surgical procedures to reduce risk of anastomotic leakage, reoperation, and surgical site infection in colorectal cancer surgery: a retrospective cohort study of 1189 patients. Int J Colorectal Dis 2018;33:755-62. [Crossref] [PubMed]
- Masoomi H, Buchberg B, Dang P, et al. Outcomes of right vs. left colectomy for colon cancer. J Gastrointest Surg 2011;15:2023-8. [Crossref] [PubMed]
- Lee KH, Ho J, Akmal Y, et al. Short- and long-term outcomes of intracorporeal versus extracorporeal ileocolic anastomosis in laparoscopic right hemicolectomy for colon cancer. Surg Endosc 2013;27:1986-90. [Crossref] [PubMed]
- Hellan M, Anderson C, Pigazzi A. Extracorporeal versus intracorporeal anastomosis for laparoscopic right hemicolectomy. JSLS 2009;13:312-7. [PubMed]
- Scatizzi M, Kroning KC, Borrelli A, et al. Extracorporeal versus intracorporeal anastomosis after laparoscopic right colectomy for cancer: a case-control study. World J Surg 2010;34:2902-8. [Crossref] [PubMed]
- Shapiro R, Keler U, Segev L, et al. Laparoscopic right hemicolectomy with intracorporeal anastomosis: short- and long-term benefits in comparison with extracorporeal anastomosis. Surg Endosc 2016;30:3823-9. [Crossref] [PubMed]
- McKenzie S, Baek JH, Wakabayashi M, et al. Totally laparoscopic right colectomy with transvaginal specimen extraction: the authors’ initial institutional experience. Surg Endosc 2010;24:2048-52. [Crossref] [PubMed]
- Akamatsu H, Omori T, Oyama T, et al. Totally laparoscopic sigmoid colectomy: a simple and safe technique for intracorporeal anastomosis. Surg Endosc 2009;23:2605. [Crossref] [PubMed]
- Vergis AS, Steigerwald SN, Bhojani FD, et al. Laparoscopic right hemicolectomy with intracorporeal versus extracorporeal anastamosis: a comparison of short-term outcomes. Can J Surg 2015;58:63-8. [Crossref] [PubMed]
- Trastulli S, Coratti A, Guarino S, et al. Robotic right colectomy with intracorporeal anastomosis compared with laparoscopic right colectomy with extracorporeal and intracorporeal anastomosis: a retrospective multicentre study. Surg Endosc 2015;29:1512-21. [Crossref] [PubMed]
Cite this article as: Brady MT. The advantage of intracorporeal techniques. Ann Laparosc Endosc Surg 2019;4:12.


