Intra-abdominal insufflation as a diagnostic modality for penetrating anterior abdominal wall trauma in a busy urban center: a retrospective case-series
Introduction
The workup and management of penetrating abdominal trauma has changed greatly over the years as technical advances and outcome research have improved our injury detection modalities, and treatment options. Management protocols have improved drastically since the 19th century when nearly all penetrating injuries were controlled non-operatively (1). It was not until WWI that we experienced our first major shift in our approach to penetrating abdominal wounds when surgeons observed higher rates of survival amongst soldiers who were treated with laparotomy (2,3). Due to the improved outcomes at that time, mandatory laparotomy became the standard treatment for penetrating abdominal wounds and remained that way until this notion was challenged in the 1960s (4). Shaftan and colleagues noticed that the rote practice of laparotomy for trauma (including non-therapeutic) resulted in a great deal of morbidity such as longer hospital stay, postoperative ileus, increased pain, wound infection, and hernias (5). Their studies inspired a movement to improve the management of abdominal penetrating wounds with more focused assessment and more selective intervention.
Following Shaftan’s work, many others over the years began to focus their efforts on establishing protocols that relied more on clinical signs and symptoms rather than on the mechanism of injury. Vital to the successful reduction in non-therapeutic intervention in these protocols was the improvement in the stratification of patients that required laparotomy from those that did not. Currently, the Eastern Association for the Surgery of Trauma (EAST) advises as a level 1 recommendation that “a routine laparotomy is not indicated in hemodynamically stable patients with abdominal stab wounds without signs of peritonitis or diffuse abdominal tenderness” (4). Non-operative management includes the use of local wound exploration (LWE) looking for defects in the fascia, diagnostic peritoneal lavage, ultrasound, CT scan and serial abdominal exams with close observation. Our ability to successfully identify and manage the stable patients with penetrating abdominal trauma is an ongoing challenge and ultimately the reason behind this study.
In our study, we propose an addition to the algorithm for the treatment of anterior abdominal stab wounds (AASW) in order to more quickly, accurately and cost-effectively evaluate the need for further intervention. Despite our current technologies and the use of LWE, focused abdominal sonography for trauma (FAST), CT scan (CT), and diagnostic laparoscopy (DL), the present-day algorithms for hemodynamically stable AASW patients without obvious peritoneal signs or eviscerations, can still result in non-therapeutic laparotomy rates of up to 82% (5) due to the fact that hollow viscous organ and diaphragmatic injuries are not accurately identified.
In this study, we aim to describe a clinical sign that can be used to assist the Trauma and Acute Care surgeon in making the diagnosis of intra-abdominal penetration. Once the correct diagnosis is made, further management decisions can be made by the surgeon depending on his or her comfort level with the minimally invasive approach.
Methods
Eight patients from December 2013 to June 2014 admitted to our level 1 trauma center were included in this study. Each patient presented to NYU Lutheran Medical Center in Brooklyn, NY, USA, after sustaining penetrating AASW.
Criteria for inclusion in this study were adults with low velocity AASW. The anterior abdomen was defined as an injury between the borders of the subcostal margins superiorly, the anterior axillary lines laterally, and the inguinal ligaments inferiorly. All eight patients were 17 years old or older and had BMIs greater than or equal to 25. All AASW in our study were from knife injuries to the anterior abdomen. Patients excluded from this study were those who were hemodynamically unstable in the trauma bay, had a history of a previous laparotomy, showed signs of peritonitis, evisceration, or shock requiring immediate surgical intervention.
All patients underwent some form of diagnostic modality (LWE, CT, or FAST) and all patients had positive findings on at least one of these modalities. LWE was considered positive if there was a violation of the anterior fascia found on assessment in the trauma bay. A CT scan was considered positive if the peritoneum was clearly violated or there was free fluid seen. FAST scan was considered positive if there were any signs of free fluid. These patients were considered candidates for DL according to the current protocol at our Trauma center.
The patients were brought to the operating room, underwent anesthesia, were prepped and draped or laparotomy, and insufflation test was performed. An insufflation test was considered positive if there was an inability to reach the target pressure of 15 mmHg upon abdominal insufflation using a Veress needle, or if the surgeon could visibly see or hear CO2 air escaping for the stab wound.
The cases were reviewed retrospectively noting peritoneal penetration utilizing DL and then comparing it with the insufflation test. After making the diagnosis of a peritoneal defect, the DL then became therapeutic or was converted to exploratory laparotomy (EL) based on surgeon comfort level with therapeutic laparoscopy. The sensitivity, specificity, positive predictive value, and negative predictive values of the abdominal insufflation test were then retrospectively calculated.
Results
From December 2013 to June 2014, eight patients with AASWs were evaluated. The demographics of each patient in the study are listed in Table 1. All eight patients were males age 17 years and older with a BMI of 25 or above. The mean age was 30 years old. All the AASW were caused by knives and all patients had only a single AASW. Mean length of stay (LOS) in the hospital was 2.75 days.
Table 1
| Patient | Age | Gender | BMI | LOS |
|---|---|---|---|---|
| 1 | 18 | M | 25.1 | 1 |
| 2 | 26 | M | 33 | 1 |
| 3 | 42 | M | 33.5 | 2 |
| 4 | 55 | M | 27.7 | 5 |
| 5 | 17 | M | 29.4 | 3 |
| 6 | 20 | M | 25.2 | 2 |
| 7 | 28 | M | 34.9 | 6 |
| 8 | 37 | M | 25.8 | 2 |
LOS, length of stay.
We compared the findings of the initial diagnostic modality with the operative findings (Table 2). Five of the eight patients were found to have positive findings of anterior abdominal wall fascia violation upon LWE. However, only four of the five patients were found to have a subsequent positive abdominal insufflation test and a positive DL. Two of the eight patients were found to have a positive FAST scan in the trauma bay and both patients were found to have subsequent positive abdominal insufflation and positive DL. Four of the eight patients were found to have positive or suspicious findings on CT scan. However, only two of the four patients were found to have subsequent positive abdominal insufflation exams and positive findings upon DL.
Table 2
| Patient # | LWE | FAST | CT scan | Abdominal insufflation | Diagnostic lap | Post sheath violation | Finding |
|---|---|---|---|---|---|---|---|
| 1 | + | − | + | + | + | + | Peritoneal violation |
| 2 | + | − | − | − | − | − | No injury |
| 3 | − | − | + | − | − | − | No injury |
| 4 | + | − | − | + | + | + | Small bowel lac |
| 5 | − | − | + | + | + | + | Small bowel lac |
| 6 | − | − | + | − | − | − | No injury |
| 7 | + | + | − | + | + | + | Liver laceration |
| 8 | + | + | − | + | + | + | Omental hematoma |
+, test performed; −, test not performed, N/A. LWE, local wound exploration; FAST, focused abdominal sonography for trauma; CT, computed tomography.
All patients with positive abdominal insufflation tests were found to have a violation of the peritoneum with or without intra-abdominal injury found on DL. Upon intra-abdominal insufflation using a Veress needle to a target pressure of 15 mmHg, all patients with peritoneal violations (5) had visible or audible CO2 escape from their wound. All patients without a violation did not have CO2 escape. We found the abdominal insufflation test to be both 100% sensitive and specific with 100% PPV and NPV for diagnosing peritoneal violation. All patients with negative insufflation test and negative DL were then extubated and subsequently discharged. The remaining five patients with positive insufflation test and DL underwent therapeutic laparoscopy with conversion to EL.
Discussion
The protocol for evaluating and managing AASW has changed dramatically since the first proposed algorithm. However, the current screening tests to determine peritoneal violation, including FAST exams, CT, and LWE have their limitations. As shown in our study along with others, the sensitivity and specificity of these exams are not accurate enough to determine peritoneal violation when compared to DL. We have evolved the algorithm to become less invasive, quicker, and more cost effective with less morbidity to the patient. According to our results, Veress needle insufflation was an accurate sign in ruling in or ruling out peritoneal violation.
In the study performed by Biffl et al., the Western trauma protocol which uses serial clinical exams and avoids the use of unnecessary tests to rule out peritoneal violation was studied. These authors also found LWE, CT, FAST and diagnostic peritoneal lavage (DPL) to not be accurate enough to rule out peritoneal injury. Instead patients were admitted and monitored with serial physical exams and vital signs to assess for clinical deterioration and further intervention (6). One of the limitations of observation with serial abdominal exam is that the patient should ideally be monitored hourly by the same doctor which is difficult to achieve in a busy center in the era of the patient “handoff”.
Some complications of Veress needle insufflation are the risks associated with general anesthesia and pneumoperitoneum including tension pneumothorax, gas embolization, iatrogenic injury, and trocar site hernia all of which are also seen with DL (7,8). Veress needle insufflation, however, allows for a smaller single incision 5 mm camera port into the abdomen which reduces the risks of infection, bleeding, and hernia as opposed to multiple sites with larger trocars used in DL. Major injury, including vascular and bowel, have been shown to have similarly low incidences when comparing Veress insufflation to the open Hasson technique, thus making the Veress approach a safe one (9).
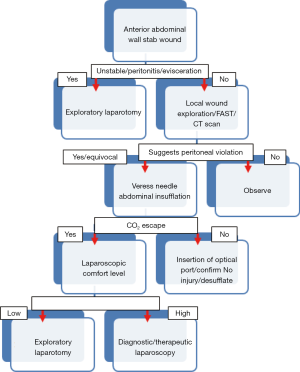
The Veress needle insufflation test can be used as a diagnostic test to rule in peritoneal violation when utilized by surgeons who do not have the advanced laparoscopic skills to perform a full DL. If the Veress needle insufflation test is positive, the surgeon without advanced laparoscopic skills will have enough evidence that posterior abdominal fascia was violated. Using this information, this surgeon can then proceed straight to EL without subjecting the patient to increased operative time and risk of insertion of the other ports needed for DL. The surgeon with more advanced laparoscopic skills who performs a positive Veress needle test can then place more ports and proceed to formal DL, therapeutic laparoscopy, or trauma EL. In the case that the Veress needle insufflation test is negative, the surgeon can place a laparoscopic camera and confirm that posterior abdominal fascia was not violated with increased certainty. A proposed addition to the current management algorithm can be seen in Figure 1. Placement of a camera port, even if the insufflation test is negative, is absolutely necessary in our eyes to serve two purposes. First, it is imperative to confirm that the peritoneum was not violated by a small caliber object such as an ice pick which could theoretically give a false negative insufflation result. Second, the port is needed to evacuate all of the pneumoperitoneum once the procedure is done so as not to have unnecessary abdominal distention and patient discomfort.
The current study has some limitations. The population in this study is very small. The sensitivity and specificity of the abdominal insufflation test would have to be assessed in a larger population in order to determine its true accuracy. False negatives are likely to occur in patients that have had prior abdominal surgery or any other reason for intra-abdominal adhesions. The retrospective design of this study also allows for recall bias on the part of the surgeon’s assessment of air escaping from the AASWs. Further prospective testing would help to confirm the accuracy of our findings.
In conclusion, our study establishes that the abdominal insufflation test along with the use of other diagnostic tests, such as FAST exams, CT scans, and LWE is highly effective in diagnosing peritoneal violations in AASWs. The abdominal insufflation test appears to be highly sensitive and specific for diagnosing peritoneal violation and may be a useful sign in the algorithm of evaluating AASWs. Utilizing this sign to help evaluate for posterior abdominal fascial penetration, the acute care surgeon can plan further intervention with greater certainty.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/ales.2017.02.28). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). This manuscript was submitted to the IRB committee and was deemed as not needing IRB approval as well as not needing informed consent due to this manuscript being a retrospective chart review.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Loria FL. Historical aspects of penetrating wounds of the abdomen. Surg Gynecol Obstet 1948;87:521-49. [PubMed]
- Pruitt BA Jr. Combat casualty care and surgical progress. Ann Surg 2006;243:715-29. [Crossref] [PubMed]
- Biffl WL, Kaups KL, Pham TN, et al. Validating the Western Trauma Association algorithm for managing patients with anterior abdominal stab wounds: a Western Trauma Association multicenter trial. J Trauma 2011;71:1494-502. [Crossref] [PubMed]
- Como JJ, Bokhari F, Chiu WC, et al. Practice management guidelines for selective nonoperative management of penetrating abdominal trauma. J Trauma 2010;68:721-33. [Crossref] [PubMed]
- Shaftan GW. Indications for operation in abdominal trauma. Am J Surg 1960;99:657-64. [Crossref] [PubMed]
- Sanei B, Mahmoudieh M, Talebzadeh H, et al. Do patients with penetrating abdominal stab wounds require laparotomy? Arch Trauma Res 2013;2:21-5. [Crossref] [PubMed]
- Fabian TC, Croce MA, Stewart RM, et al. A prospective analysis of diagnostic laparoscopy in trauma. Ann Surg 1993;217:557-64; discussion 564-5. [Crossref] [PubMed]
- Sumislawski JJ, Zarzaur BL, Paulus EM, et al. Diagnostic laparoscopy after anterior abdominal stab wounds: worth another look? J Trauma Acute Care Surg 2013;75:1013-7; discussion 1017-8. [Crossref] [PubMed]
- Agresta F, De Simone P, Ciardo LF, et al. Direct trocar insertion vs Veress needle in nonobese patients undergoing laparoscopic procedures: a randomized prospective single-center study. Surg Endosc 2004;18:1778-81. [Crossref] [PubMed]
Cite this article as: Meytes V, Amaturo M, Price EE, Ferzli G, Timoney M. Intra-abdominal insufflation as a diagnostic modality for penetrating anterior abdominal wall trauma in a busy urban center: a retrospective case-series. Ann Laparosc Endosc Surg 2017;2:49.